At the beginning of the COVID-19 pandemic, the shortage of N95 respirator masks presented a dire situation for the healthcare and frontline workers who needed them most. Essential workers who relied on N95 masks had no choice but to wear what were meant to be disposable N95 masks for weeks at a time. Some started disinfecting the masks to be redistributed and reused.
Now, as COVID-19 infections surge and states such as Texas and Florida and hospitals and healthcare workers once again become overwhelmed with the volume of patients, N95 respirators still remain in short supply.
But engineers and researchers at MIT and Brigham and Women’s Hospital have a created a new type of face mask that could be a game-changer. In a laboratory setting, the prototype worked as well as a N95 respirator at filtering out virus-containing particles.
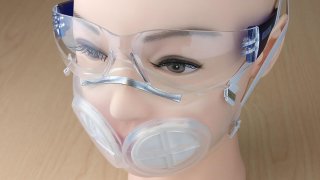
The biggest innovation? While N95 masks are made entirely from a special material that filters out airborne droplets and fluids that could contain the COVID-19 virus, the new MIT mask is made from silicone, with slots for just two small, disposable disks of the N95 material (which serve as filters). That means the masks themselves can be quickly and easily sterilized and reused, and though the small filters must be thrown out, each mask requires much less N95 material.
More Coronavirus Pandemic Coverage
Called the iMASC, which stands for Injection Molded Autoclavable, Scalable, Conformable, this design could help solve shortage issues.
The new iMASC system can also be sterilized a few different ways without sacrificing its effectiveness, the researchers wrote in a paper published in the British Medical Journal Open. For example, researchers were able to use a steam sterilizer on the masks, put the masks in an oven, as well as soak them in both bleach and rubbing alcohol. (Treating used N95 masks with hydrogen peroxide disinfectants to neutralize any viruses requires special equipment and takes a few days. It also only allows the masks to be re-worn for one day at a time, up to 20 more times.)
The iMASC researchers "wanted to maximize the reusability of the system," Giovanni Traverso, an MIT assistant professor of mechanical engineering and a gastroenterologist at Brigham and Women’s Hospital, said in a press release.
The new mask could also be more environmentally-friendly — it uses less disposable material, which produces much less waste than tossing a whole mask, Adam Wentworth, a research engineer at Brigham and Women’s Hospital and a research affiliate at the Koch Institute, said in a press release.
So far, the masks have proven effective and comfortable.
A group of 24 healthcare workers (including nurses, physicians and technicians) wore the new masks and completed tests that involved breathing, talking, moving their head and body and making facial expressions. The participants said that the mask fit well and felt breathable. Most importantly, the mask successfully filtered out a sugar solution in the air that was used to mimic aerosolized respiratory droplets.
More tests need to be done, and the group is currently working on a second mask design.
The team plans to eventually have the rubber mask approved by the Food and Drug Administration and the National Institute for Occupational Safety and Health. Once complete, the masks could cost hospitals $15 each, Fast Company reported. (N95 masks can cost between $2.80 and $6.95 per unit, according to data compiled by nonprofit Project N95.)
The ultimate goal is to make the masks available for healthcare workers as well as the general public, but there is no timeline as of yet.



