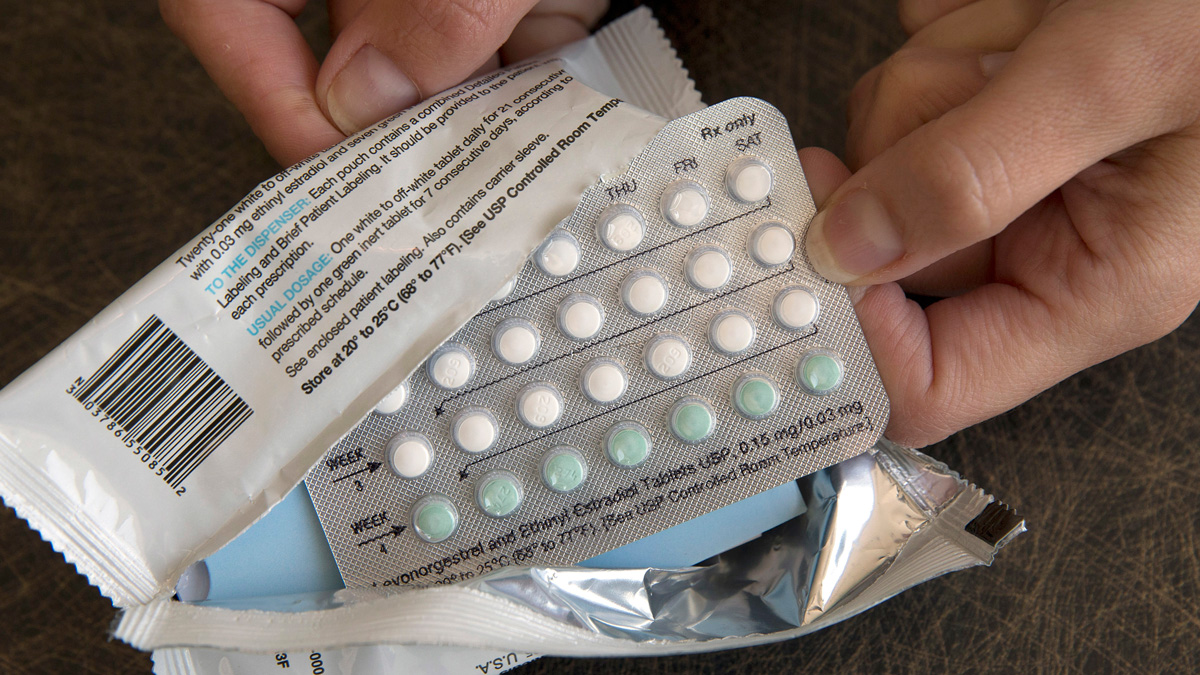
Studies have suggested for decades that birth control pills containing both estrogen and progestogen — synthetic versions of female hormones — may slightly elevate one’s risk of breast cancer. But less research has focused on the risk associated with progestogen-only contraceptives like intrauterine devices or the so-called mini pill.
A study published Tuesday, March 21, in the journal PLOS Medicine found that the risk of developing breast cancer is similar across all of these options, whether they rely on one hormone or two.
The relative risk of being diagnosed with breast cancer was 20% to 30% higher among women who use or recently used birth control pills with a two-hormone combination, progestogen-only pills or hormonal IUDs compared to women who did not.
As of 2019, 14% of U.S. women ages 15 to 49 took oral contraceptive pills, and around 10% used long-acting reversible contraceptives such as IUDs or birth control implants, according to the Centers for Disease Control and Prevention.
We're making it easier for you to find stories that matter with our new newsletter — The 4Front. Sign up here and get news that is important for you to your inbox.
“I really don’t want women to be seeing this and thinking, ‘Oh, no, I’ve got to come off the progestogen-only pill,’” said Gillian Reeves, who co-authored the new study and directs the Cancer Epidemiology Unit at the University of Oxford.
“There is this increased risk whatever you use in terms of hormonal contraceptives,” she added. “These newer types that hadn’t been so well studied, what it does look like is that they are certainly no worse.”
The findings are based on an analysis of prescription records from women under age 50 in the U.K. Nearly 9,500 of those women were diagnosed with breast cancer between 1996 and 2017, while more than 18,000 were not.
The researchers combined the results of their analysis with findings from 12 other studies that examined the risk of progestogen-only contraceptives. The overall results were similar, suggesting that hormonal contraception could raise the risk of breast cancer by up to 30%.
This is relative risk, however: The average woman has a 1-in-8 chance of developing breast cancer at some point in her life, so the study suggests that hormonal birth control slightly ups those odds.
Among women ages 35 to 39, Reeves said, “we estimate that the extra risk is only going to be (in) the order of about 0.2% over that 15-year period, so it is still relatively small.”
Dr. Rachel Urrutia, an associate professor of obstetrics and gynecology at the University of North Carolina School of Medicine, said the new findings are consistent with other similar studies. Her own 2013 analysis, she added, found that birth control pills with a two-hormone combination increased breast cancer rates by around 8%.
But Urrutia, who wasn’t involved in the new research, said that it’s difficult to conclude with certainty that hormonal contraception raises the risk of cancer without conducting a randomized controlled trial.
“That’s going to be hard to do for birth control pills, because you can’t always find people who are willing to be randomized to take birth control pills or not take them,” she said.
She added that it’s possible that the increased risk of breast cancer in Reeves’ study and others could be linked to other factors. Diet or a family history of breast cancer may also influence risk, Urrutia said, and Reeves’ study did not adjust for those particular variables.
Breast cancer risk could decline after stopping birth control
Reeves’ analysis included a study from 2017 that similarly identified a 20% increased risk of breast cancer among women who had currently or recently used hormonal contraception.
That study followed 1.8 million women in Denmark for more than 10 years, on average. For every 7,690 women using hormonal contraception for a year, there was one additional case of breast cancer relative to women who never used hormonal contraception.
Reeves said breast cancer is hormone-sensitive: Estrogen and progesterone can activate hormone receptors in cancer cells, which may stimulate the growth of those cells.
“Anything that you give to a woman that disrupts her normal menstrual cycle has the potential to change her exposure to both of these sex hormones, and in doing so, it may well change her risk of hormonally sensitive cancers,” she said.
But once a person stops using hormonal birth control, Reeves added, the bulk of research indicates that the risk of breast cancer gradually declines.
“We wouldn’t expect that use 10, 15 years ago is going to have much effect currently,” she said.
Urrutia said more research is needed before doctors can advise patients about how birth control affects their cancer risk over time, even after stopping it.
Some past studies have even found that hormonal contraception can decrease the risk of some other forms of cancer, according to the National Cancer Institute. That list includes endometrial, ovarian and colorectal cancers.
“Given that the protection against ovarian and endometrial cancer is quite a bit more substantial and it lasts for longer — it lasts into middle age, when those cancers start becoming much more common — I would say that for most women, the benefits will probably outweigh the risk of breast cancer,” Reeves said.
This story first appeared on TODAY.com. More from TODAY: