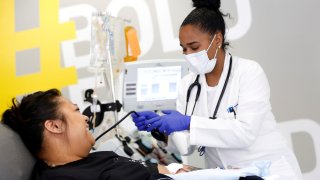
- The WHO's Guideline Development group found that "there was no clear benefit for critical outcomes such as mortality and mechanical ventilation."
- Convalescent plasma therapy gives Covid patients a transfusion of blood plasma from someone who has recovered from the virus in the hope the donor's antibodies will help fight the infection.
- The U.S. Food and Drug Administration scaled back its convalescent plasma emergency use authorization in February.
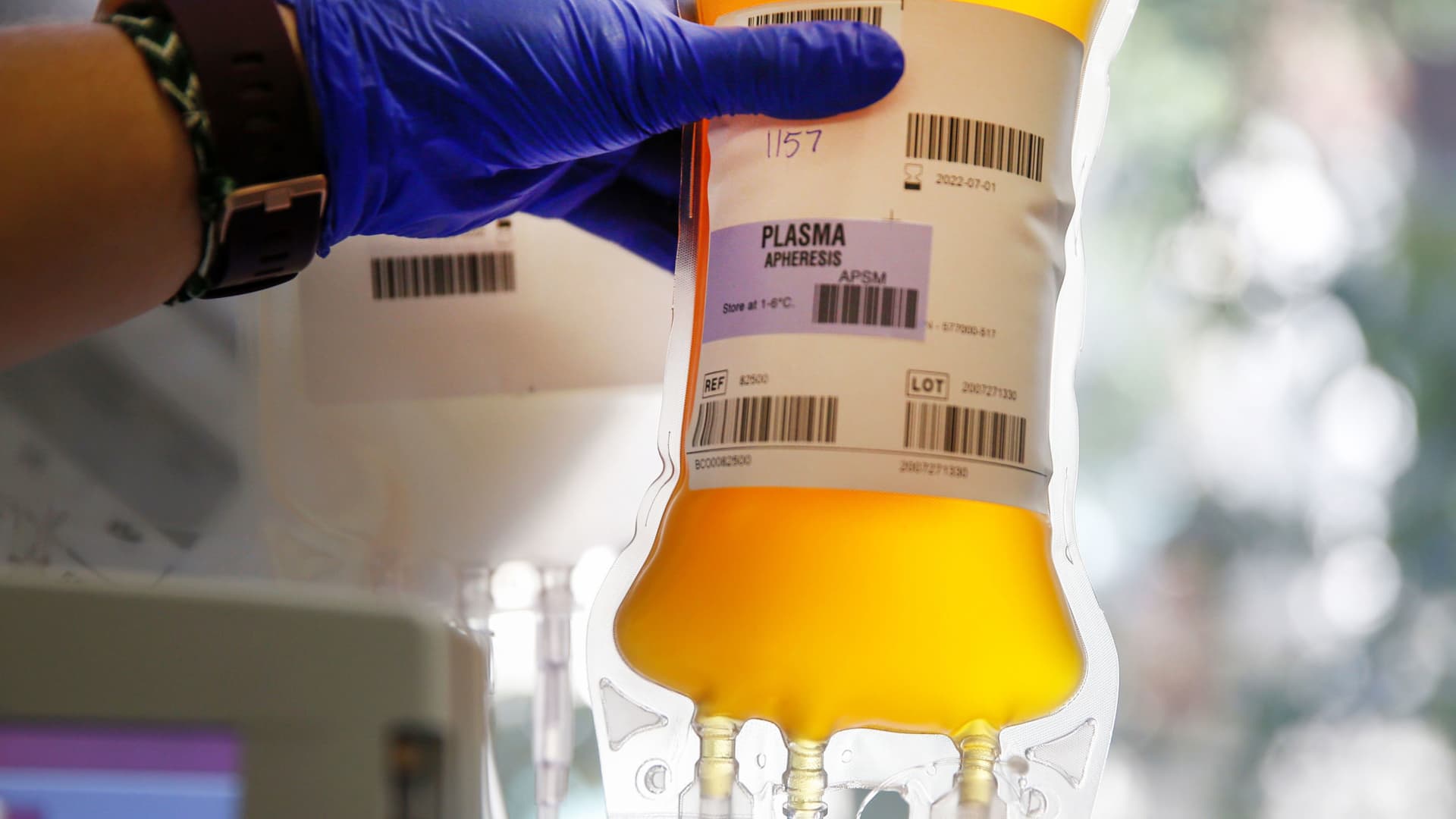
The World Health Organization on Monday issued a strong recommendation against administering convalescent plasma to treat Covid-19 patients, citing research that shows no improvement in patients who received the treatment.
In convalescent plasma therapy, blood plasma is donated by someone who has recovered from the virus and transferred into a patient battling the virus with the hope the donor's antibodies help fight the infection.
We're making it easier for you to find stories that matter with our new newsletter — The 4Front. Sign up here and get news that is important for you to your inbox.
However, the WHO's guideline development group found that "there was no clear benefit for critical outcomes such as mortality and mechanical ventilation for patients with non-severe, severe or critical illness, and significant resource requirements in terms of cost and time for administration."
The group said the treatment also faces practical challenges, such as finding and testing donors as well as collecting, storing and transporting the plasma.
The recommendation is based on 16 trials with more than 16,000 patients with non-severe, severe and critical Covid infections. The group said research on the treatment should proceed in randomized control trials. The new recommendation is published in the British Medical Journal.
Money Report
The U.S. Food and Drug Administration in February scaled back its convalescent plasma emergency use authorization to cover only hospitalized patients early in disease progression and those hospitalized who have immune system disorders in which they cannot produce a strong antibody response.
"Plasma with low levels of antibodies has not been shown to be helpful in COVID-19," the FDA said in its revised emergency authorization in February.
The agency issued its original, broader authorization on an emergency basis in the U.S. for all hospitalized patients in August 2020 when there were no other approved treatments for the virus. During the Trump administration, Health and Human Services Secretary Alex Azar had celebrated the use of convalescent plasma at the time as a "milestone achievement" in the efforts to fight Covid.
Since then, the FDA has authorized two Covid treatments: Gilead's antiviral drug remdesivir in October 2020 and Regeneron's antibody cocktail the following month. Pfizer's two-dose vaccine was authorized about a year ago.
The National Institutes of Health in August also said convalescent plasma didn't help patients in an NIH-backed study of more than 500 adult Covid patients at the University of Pittsburgh. The trial was stopped in February due to its lack of effectiveness, the NIH said.
The New England Journal of Medicine, in a study published last month, found that convalescent plasma did not prevent disease progression in high-risk outpatients when administered one week after symptom onset. It also did not improve clinical outcomes in hospitalized patients late in the course of their illness, according to the study.
However, the study found that convalescent plasma did reduce disease progression in older, outpatient adults if administered within 72 hours of symptom onset.
Pfizer and Merck are now seeking emergency use authorization for oral antiviral drugs designed to reduce the risk of hospitalization from Covid.






